- Bacterial Vaginosis is the dysbiosis of the vaginal microbiome characterized by foul-smelling, thin white discharge, and high vaginal pH (> 4.5).
- Pelvic Inflammatory Disease is the infection of reproductive organs in females caused as a result of bacteria traveling up from the vagina to the uterus, fallopian tubes, and ovaries.
- PID is characterized by pain in the pelvic region, pain while having intercourse, or unusual vaginal discharge and bleeding.
- Women suffering from recurrent BV or chronic untreated BV might have an increased risk of contracting PID.
- These infections might lead to complications such as the increased risk of developing STIs, pregnancy-related complications, or even infertility.
- Avoiding multiple sex partners, unprotected sex, over-cleaning, or douching might help in preventing these infections.
- Natural remedies such as the use of probiotics, prebiotics, garlic, and greek yogurt, and not only helps in preventing these infections but also boost your immunity against them.
Sometimes specific health problems tend to be associated with others. Having one problem can increase the risk of acquiring another. Such is the association between Bacterial Vaginosis (BV) and Pelvic Inflammatory Disease (PID).
Although not much research has been conducted on this topic, still a casual relationship has been seen between the two. Let us first get to know what BV and PID are.
Bacterial Vaginosis (BV) – dysbiosis of the vaginal microbiome
Bacterial Vaginosis is a type of infection or inflammation of the vagina (vaginitis), as told by experts at Mayo Clinic. It is characterized by a disturbance in the balance of natural flora in the vaginal environment.
When there is a deficiency of good bacteria in the vagina, the environment becomes feasible for bad bacteria to grow. This results in an infection called Bacterial Vaginosis. (1)
What are the symptoms of Bacterial Vaginosis (BV)?
According to a report from UpToDate. an evidence-based clinical resource, about 85% percent of women with Bacterial Vaginosis experience no symptoms. However, the remaining percentage of women do experience some specific symptoms associated with Bacterial Vaginosis.
These are some of the symptoms of Bacterial Vaginosis (BV) which are as follows:
- Abnormal vaginal discharge.
Women with Bacterial Vaginosis may notice a change in the color of their vaginal discharge. Usually, vaginal may be milky white in color, but with Bacterial Vaginosis, the color of the discharge may change to grayish. The discharge may also become thin and watery. To learn more about your vaginal discharge you can check out our article on the different types of vaginal discharge. - Abnormal vaginal odor.
Bacterial Vaginosis also manifests itself as an abnormal vaginal odor that may be foul and unpleasant. - Change in vaginal pH.
Normally, the pH of a healthy vagina is lower than 4.5 as the vaginal environment is naturally acidic. However, in the case of Bacterial Vaginosis, the vaginal pH rises and becomes greater than 4.5. To learn more about your vagina’s pH you can dig deeper into why your pH levels are important. - Burning and irritation.
Although this is not a symptom associated with Bacterial Vaginosis, burning, and irritation in the genital area may occur in the case of Bacterial Vaginosis. (2)
Pelvic Inflammatory Disease (PID)
According to the CDC, pelvic inflammatory disease is an upper genital tract infection in females. It occurs when sexually transmitted bacteria move from the vagina, which is the lower genital tract to the uterus, ovaries, and fallopian tubes, which is the upper genital tract. This disease mostly occurs in females who are sexually active, which are between the ages of 15 and 48.
What are the symptoms of Pelvic Inflammatory Disease (PID)?
Pelvic Inflammatory Disease manifests itself in the form of the following symptoms, as reported by the NHS:
- Pelvic pain (around the lower abdomen.)
Light to mild pain in the stomach or lower abdomen. - Unusual vaginal bleeding.
Longer, heavier, painful periods or spotting throughout your menstrual cycle. - Pain during sexual intercourse.
Discomfort/pain during or after intercourse - Unusual vaginal discharge.
Yellow or greenish in color and has an unusual odor. - Painful urination.
Pain, burning sensation, or discomfort while urinating. - Nausea.
Feeling nauseous, loss of appetite, and/or vomiting. - Fevers.
Low-grade fevers that come and go, or sudden high-grade fevers with chills.
What are the complications of PID?
- Tubo-ovarian abscess (TOA):
a pocket of pus that forms because of an infection in a fallopian tube and ovary. - Tubal factor infertility:
happens when diseases, damage, scarring, or obstructions in the fallopian tubes prevent the sperm from reaching the ovary to fertilize an egg or prevent a fertilized embryo from reaching the uterus for pregnancy. - Ectopic pregnancy:
A pregnancy in which the fertilized egg implants outside the uterus. An untreated ectopic pregnancy can cause serious complications for mother and baby. - Chronic pelvic pain:
pelvic pain that persists for 6 months or longer in the area below your belly button and between your hips.
What are the risk factors for PID?
The risk factors for developing PID are being younger, the use of an intrauterine device (IUD), having new or multiple sexual partners, douching, having unprotected sex, and having a history of STD’s.
How is PID diagnosed?
There isn’t a particular test to diagnose PID. However, your doctor will follow a protocol of a series of findings to evaluate if you have PID.
- Medical history.
Your doctor will ask about your history of any sexually transmitted diseases, birth control methods, and sexual activity. - Signs and symptoms of PID.
Make sure to inform your doctor about any symptoms that you might be experiencing. Nothing is too small, so make sure to not leave anything out. - Pelvic exam.
During your visit, your doctor will likely do a pelvic exam. Your doctor may look for a change in discharge, swelling, and take cotton swabs to test for different infections. - Ultrasound.
This test might be done to check your reproductive organs.
Does BV cause PID?
According to a study conducted by Taylor et al. in 2013, Bacterial Vaginosis associated organisms such as Gardnerella vaginalis and Mycoplasma hominis can cause damage to reproductive organisms. In humans, these organisms have been seen to cause reproductive health problems like endometritis (inflammation of the inner lining of the uterus) and salpingitis (inflammation of fallopian tubes). This means that BV can also be associated with Pelvic Inflammatory Disease.
Bacterial Vaginosis is usually characterized by a deficiency of the good bacteria ‘lactobacillus,’ which prevents bad bacteria from causing infections. Thus, in the absence of lactobacillus, the body becomes vulnerable to infection. Therefore, this concludes that the presence of Bacterial Vaginosis can make a person susceptible to acquiring STDs resulting in Pelvic Inflammatory Disease. (4)
What is the difference between Bacterial Vaginosis and Pelvic Inflammatory Disease?
BV and PID differ in certain ways which are as follows:
- BV is an infection of the lower genital tract, whereas PID is an infection of the upper genital tract.
- BV is caused by a deficiency of good bacteria in the vaginal environment, whereas PID is caused by the presence of sexually transmitted bacteria.
What are the complications associated with BV?
Most of the time, Bacterial Vaginosis does not cause serious health problems, but sometimes it can cause chronic health issues if neglected.
Here are some of the complications which can result from Bacterial Vaginosis:
- Complications in pregnancy.
Pregnant women with Bacterial Vaginosis are at a high risk of premature births and low birth weight of their babies. - Increased risk of Sexually Transmitted Infections (STIs).
Women with Bacterial Vaginosis are at a higher risk of acquiring sexually transmitted infections such as HIV, chlamydia, and gonorrhea. This is because they have a deficiency of good bacteria that fight infection, thus making the body susceptible to infections. - Pelvic Inflammatory Disease.
As described above, the occurrence of Bacterial Vaginosis can also increase the risk of acquiring Pelvic Inflammatory Disease. (5)
How to prevent PID and BV?

Problems like Bacterial Vaginosis and PID can be life-threatening at times. They can cause not only temporary health problems but chronic health issues as well. So, it is best to take some preventive measures to avoid the occurrence of these problems
Here are some of the preventive measures you can take to dodge these infections:
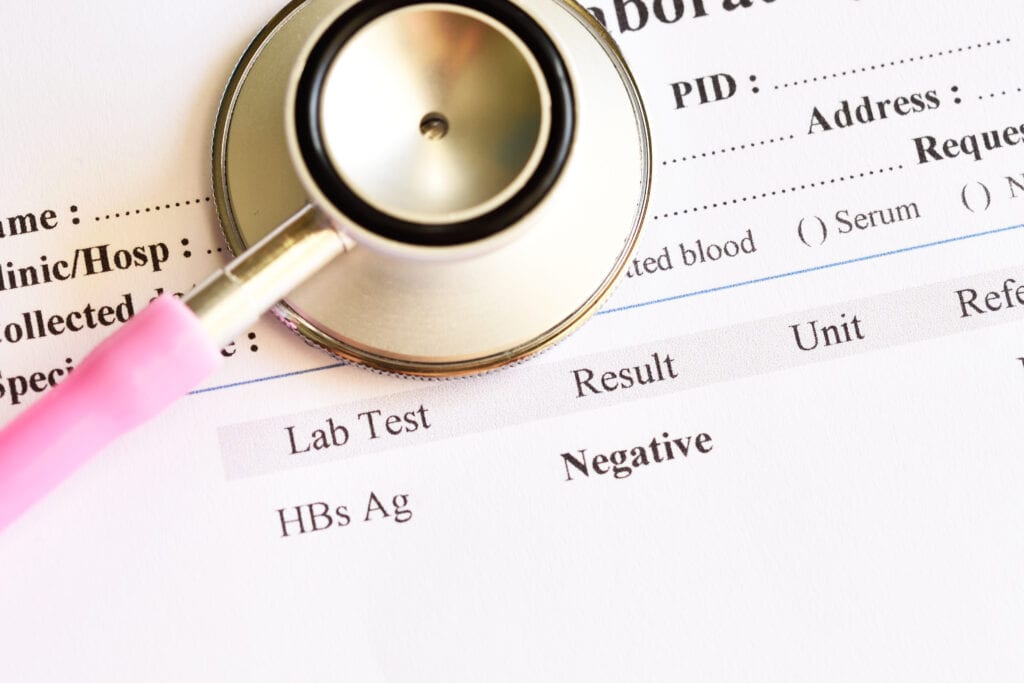
1. Frequent testing for STIs
Get yourself frequently tested for the presence of any sexually transmitted infection so that it can be treated immediately. If you are sexually active, then you must get your sex partner to get tested as well.
2. Try Vaginal Probiotics
Probiotics encourage the gut and vaginal microbiome to grow the “good” bacteria that help fight off the “bad” bacteria. Eating foods full of probiotics like yogurt and/or taking a probiotic supplement might help prevent BV and PID (7)
3. Avoid using douches
Some people consider douching to be a good approach for vaginal hygiene, but it isn’t. Douches are more likely to spread an infection deeper into the genital tract, so you should avoid using vaginal douches altogether. (9)
4. Use protection during intercourse
It is imperative to take protective measures while having sex. It is preferable if your male sex partner uses a condom so that any infections are not transferred. And with female partners make sure to clean your sex toys before using them with your partners as bacteria can be transferred from partner to partner.
5. Limit the number of sex partners
Avoid having sex with different people on and off. This can upset the balance of the natural flora in your vagina and may result in infections.
Make sure to always consult with your doctor or medical provider if any of these issues persist.
- Mayoclinic, Bacterial Vaginosis (BV). Bacterial Vaginosis – Symptoms and causes
- UpToDate, Patient education, Bacterial Vaginosis (beyond the basics). Bacterial Vaginosis – Beyond the basics
- National Health Services, UK. Pelvic Inflammatory Disease (PID). Overview – Pelvic inflammatory disease
- Taylor, B. D., Darville, T., & Haggerty, C. L. (2013). Does Bacterial Vaginosis cause pelvic inflammatory disease?. Sexually transmitted diseases, 40(2), 117-122.
- International Society of Sexual Medicine (ISSM), What are possible complications for Bacterial Vaginosis?. What are possible complications for bacterial vaginosis? | ISSM
- Mayoclinic, Pelvic Inflammatory Disease (PID). Pelvic inflammatory disease (PID) – Symptoms and causes
- Al‐Ghazzewi, F. H., & Tester, R. F. (2016). Biotherapeutic agents and vaginal health. Journal of applied microbiology, 121(1), 18-27.
- Bilardi, J., Walker, S., McNair, R., Mooney-Somers, J., Temple-Smith, M., Bellhouse, C., … & Bradshaw, C. (2016). Women’s management of recurrent Bacterial Vaginosis and experiences of clinical care: a qualitative study. PLoS One, 11(3).
- Wan, B. P., & Jacobs, C. K. (2018). Does vaginal douching cause Bacterial Vaginosis?. Evidence-Based Practice, 21(6), 13.





