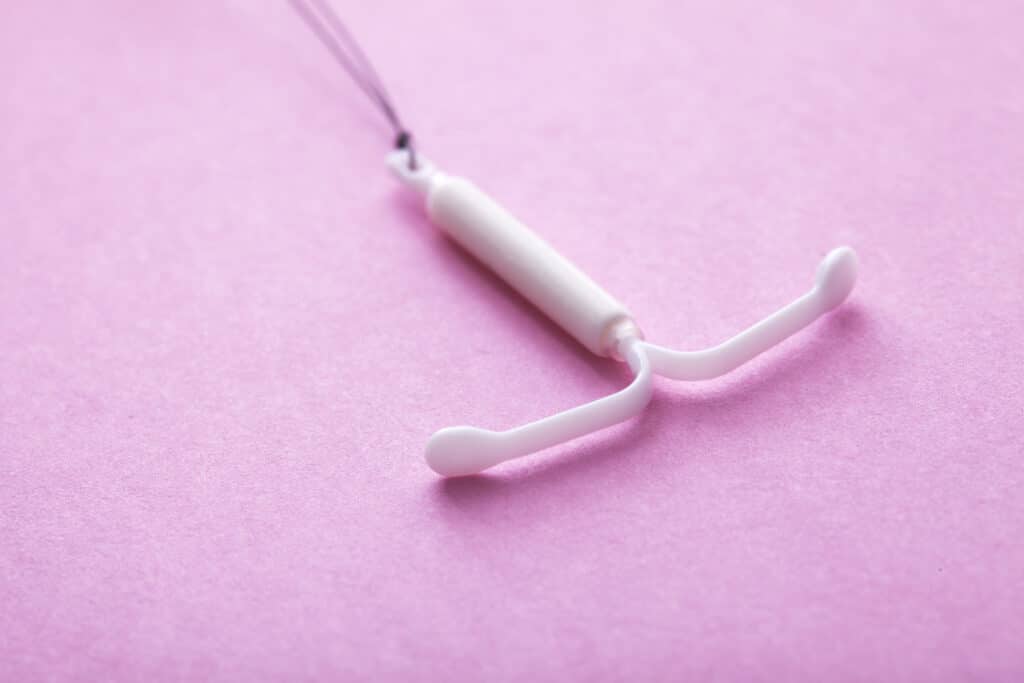
- Intrauterine devices are small T-shaped contraceptive devices meant to be placed in your uterus.
- The U.S. has four approved IUDs i.e. 1 non-hormonal copper-bearing and 3 hormone-based.
- IUDs have 99% efficacy and are safe to use, however, they might disrupt your vaginal microbiome.
- IUDs may increase the chances of vaginal infections such as Bacterial Vaginosis (BV) and yeast infections.
- BV can be prevented by practicing good hygiene, using probiotics, avoiding multiple sex partners, and discontinuing chemical and fragranced products.
Intrauterine devices are becoming more popular among women searching for problem-free contraceptive options. Their popularity is based on how easy they are to use, their 99% efficacy, and fewer to no side effects.
However, some women who have IUDs may experience irregular bleeding patterns, unusual odors with copper options, and in some cases vaginal infections.
When Irregular bleeding patterns occur, the vaginal pH may increase, making you more vulnerable to vaginal infections such as bacterial vaginosis and STIs.
What are Intrauterine contraceptive devices (IUDs)?
Intrauterine devices are small T-shaped contraceptive devices made of copper meant to be placed within the uterus. IUDs are very effective as compared to other contraceptive methods such as pills and condoms. (1)
According to the CDC, IUDs are 99% effective. 1 out of 100 women may get pregnant within the first year of using the device. Placing a copper device might sound very invasive and painful but once placed you don’t feel anything.
In the US, there are four IUDs approved for contraceptive purposes. One non-hormonal copper-bearing IUD and three levonorgestrel-releasing IUDs (hormonal).
How different types of IUDs work?
- Copper-bearing IUDs are made of copper and plastic. These are non-hormonal and copper acts as a spermicide (a substance capable of killing sperms, preventing them from reaching the uterus).
- Progestin levonorgestrel-releasing IUDs cause the uterus lining to become thin and cervical mucus to become thick. Thick mucus prevents the sperm from the egg or fertilizing it. (2,3)
According to statistics of National Survey Family Growth (2018), about 10.3% of the women in the US use IUDs for contraception. These devices are most commonly used to achieve contraception with over 168 million women using it worldwide. (4)
What are the pros and cons of using IUDs?
Pros
- IUDs are effective in controlling pregnancy for the long term and the effect is reversible. Your healthcare provider can remove it safely and no surgical treatment is required for that.
- Copper bearing non-hormonal IUDs can instantly provide contraception without making your hormones go haywire.
- Unlike pills, you don’t have to keep reminding yourself that you’re on contraception. Once placed in your uterus, you will most probably forget about it.
Cons
- Some women might experience mild cramps, abdominal pain, and irregular bleeding in the first few weeks after the placement
- You might get shorter or no periods at all for a few months.
- IUDs do not provide protection against Sexually Transmitted Infections (STIs).
- IUDs might make you more prone to vaginal infections such as Bacterial Vaginosis (BV) and yeast infections by disturbing the delicately balanced vaginal microbiome. (5)
What is the vaginal microbiome?
When you are born, you are free from any micro-organisms (you’re pretty much sterile). As soon as you take your first breath you begin to develop your own unique microbiome.
What creates your microbiome is dependent on environmental conditions, your mother’s microflora, the food you eat, and various other factors. Once you grow up, your body becomes home to trillions of microbes.
The vaginal microbiome is your vagina’s unique mix of different microbes that populate it.
Almost every organ of your body hosts these microbes and good ones among them keep a strong check on bad ones. Your vagina is dominated by bacteria from Lactobacilli species.
The stability of your vaginal microbiome depends on several factors:
- Hormonal changes you experience with different contraceptives or during menstruation.
- Use of any vaginal care products such as douches, vaginal washes, and soaps, etc.
- Your sexual interactions
- Diet
- Use of medications such as antibiotics etc.
It’s good to know that your vagina is capable of self-cleaning. It produces discharge which washes off the bad bacteria and dead cells. Therefore, the powerful combination of its self-cleaning abilities, good bacteria, and local immune defense can keep your vaginal microbiome balanced. (6)
How does the vaginal microbiome work?
The vaginal microbiome is rich with many kinds of microbes. The dominant microbe is known as Lactobacillus, which produces lactic acid and hydrogen peroxide in order to maintain an acidic environment.
It’s this symbiotic relationship of probiotics keeping acidic levels maintained that keeps the probiotics thriving. And as a result, they produce compounds needed for the vagina to function properly and minimize the growth of bad bacteria. (7)
Why is it important to keep your vaginal microbiome balanced?
Good bacteria such as Lactobacilli are responsible for keeping bad bacteria at bay. Once your vagina increase pH, bad bacteria are in an optimal state to compete for prebiotics and create their toxins. This is the best working theory as to what may cause BV.
A slight shift in vaginal pH may cause drastic changes in the microbial flora. This may increase your chances of causing vaginal infections and contracting STDs. (8)
How can IUDs mess up your vaginal microbiome?
How IUDs disrupt the vaginal microbiome is quite unclear, however, evidence suggests it sure does mess up your normal microflora. Here’s how…
- One study suggests that the presence of foreign devices in the vagina can increase the number of pathogens (harmful bacteria). This makes your vagina more prone to BV.
- Secondly, women who use copper IUDs experience irregular bleeding patterns. Menstrual blood (pH 7.4) can increase the pH of your vagina which can lead to BV. (9)
How can IUDs lead to bacterial vaginosis or BV?
According to WebMD, bacterial vaginosis is an infection caused by an imbalance between good and bad bacteria residing in your vagina. Health experts call it vaginal dysbiosis which means the imbalance of normal microbiomes.
BV is known for giving off an unusual odor (what we come to relate to as a fishy smell), thin white or gray discharge, and increased vaginal pH.
If it stays untreated for a long duration, recurrent bv is probable and will lead to multiple health problems. The complications caused by chronic BV just for pregnant women alone are: preterm birth, preterm labor, low birth weight of infants, and miscarriages, etc. (10)
There might be limited evidence of how IUDs can cause BV but there is enough evidence to show that they do.
- A study was conducted to compare the prevalence of BV in women having IUDs and those who take oral contraceptives. The results showed a three-fold increased chance of BV in women having IUDs. (11)
- An article published in an Evidence-Based Practice journal concluded that women using IUDs have 7-47% more chances of contracting BV. Women on oral contraceptives, on the other hand, have 2-35% chances of contracting BV. (12)
What are the factors that may lead to BV?
You might suffer from BV as a consequence of your vaginal pH going up or when bad bacteria outgrows good ones. Bad bacteria are opportunistic in nature and as soon as they get a chance, they grow in number causing BV. According to the CDC, almost 29.2% of women in the US are suffering from BV.
The following factors may lead to BV
- Multiple sex partners – Semen has a high pH between 7.2-7.8 which can disrupt your vaginal pH and the microbial balance. Also, your sexual partner or partners have their own microbiome too, intercourse will affect yours as well.
- Douching – We cannot say it enough, please do not douche! It washes off good bacteria too, leaving you more prone to BV.
- Using fragranced or chemical-laden soaps, shampoos, and scents as these chemicals make your vaginal pH fluctuate
- Taking antibiotics too often – most antibiotics can’t differentiate between good and bad bacteria and may kill both.
What are the signs and symptoms of BV?
According to data collected by the CDC, about 85% of the women suffering from BV do not show any symptoms. However, for the rest of the women, BV symptoms can be a total nightmare.
- Vaginal discharge with an unusual odor
- Itching around the vaginal opening or vulvar area (not to confuse with the vagina or cervix)
- Burning sensation while peeing
- Thin discharge of white to a grayish color
How can your BV infection be diagnosed?
The answer is simple. If you’re experiencing any of the symptoms mentioned above, then you’ll need to consult your OB/GYN or health care provider ASAP. Amsel’s criteria are the most accepted way to diagnose BV. It has 4 parameters:
- Presence of thin and grayish-white discharge
- Positive whiff test – adding a drop of potassium hydroxide on discharge will give off a bad fishy odor
- Vaginal pH > 4.5
- Presence of clue cells
How can you prevent and treat your BV caused by IUD?
Prevention is always better than treatment. In order to minimize the likelihood of getting BV or recurring bacterial vaginosis, try the following recommendations.
- Practice good hygiene
- Avoid the use of chemicals such as soaps, shampoos, vaginal washes on your vagina.
- Opt for a healthy diet based on veggies and fruits.
- Avoid having multiple sex partners and unprotected sex
- Say no to douching because it does more bad than good
- Add probiotics to your diet. Probiotics can boost your immunity and up your good bacteria game.
If you’re not experiencing any uncomfortable symptoms of BV then treatment might not be necessary.(14,15)
- Nelson, A. L., & Massoudi, N. (2016). New developments in intrauterine device use: focus on the US. Open access journal of contraception, 7, 127.
- Centers for Disease Control and Prevention (CDC), Classification of intrauterine devices. Classifications for Intrauterine Devices
- United States Selected Medical Eligibility Criteria (US MEC) for contraceptive use, 2016, Centers for Disease Control and Prevention (CDC). Classifications for Intrauterine Devices
- Key statistics from National Survey Family Growth (NSFG). NSFG – Key Statistics from the National Survey of Family Growthl
- U.S Department of Human and Health Services, Intrauterine Devices (IUDs). Intrauterine Device (IUD)
- Ma, B., Forney, L. J., & Ravel, J. (2012). Vaginal microbiome: rethinking health and disease. Annual review of microbiology, 66, 371-389.
- Bertuccini, L., Russo, R., Iosi, F., & Superti, F. (2017). Effects of Lactobacillus rhamnosus and Lactobacillus acidophilus on bacterial vaginal pathogens. International journal of immunopathology and pharmacology, 30(2), 163-167.
- Martin, D. H. (2012). The microbiota of the vagina and its influence on women’s health and disease. The American journal of the medical sciences, 343(1), 2-9.
- Demirezen, Ş., Küçük, A., & Beksaç, M. S. (2006). The association between copper-containing IUCD and bacterial vaginosis. Central european journal of public health, 14(3).
- WebMD, Bacterial Vaginosis (BV). WebMD, Bacterial Vaginosis (BV).
- Joesoef, M. R., Karundeng, A., Runtupalit, C., Moran, J. S., Lewis, J. S., & Ryan, C. A. (2001). The high rate of bacterial vaginosis among women with intrauterine devices in Manado, Indonesia. Contraception, 64(3), 169-172.
- Sliwowska, A., & Amico, J. (2018). Is the risk of bacterial vaginosis (BV) increased in women with intrauterine devices (IUDs)?. Evidence-Based Practice, 21(7), E2-E3.
- Iavazzo, C., Gkegkes, I. D., Zarkada, I. M., & Falagas, M. E. (2011). Boric acid for recurrent vulvovaginal candidiasis: the clinical evidence. Journal of Women’s Health, 20(8), 1245-1255.
- Centers for Disease Control and Prevention (CDC), Bacterial vaginosis or BV statistics. Centers for Disease Control and Prevention (CDC),
- Bacterial vaginosis or BV statistics.
- Amsel, R., Totten, P. A., Spiegel, C. A., Chen, K. C., Eschenbach, D., & Holmes, K. K. (1983). Nonspecific vaginitis: diagnostic criteria and microbial and epidemiologic associations. The American journal of medicine, 74(1), 14-22.